RJPS Vol No: 15 Issue No: 4 eISSN: pISSN:2249-2208
Dear Authors,
We invite you to watch this comprehensive video guide on the process of submitting your article online. This video will provide you with step-by-step instructions to ensure a smooth and successful submission.
Thank you for your attention and cooperation.
1Auwal Shehu Ali, School of Allied Health Sciences, Sharda University, Greater Noida, Uttar Pradesh, India.
2Department of Biochemistry and Molecular Biology, Usmanu Danfodiyo University Sokoto, Nigeria
3Department of Biochemistry and Molecular Biology, Usmanu Danfodiyo University Sokoto, Nigeria
4Kano Drugs and Medical Consumables Supply Agency, Kano, Nigeria
5Department of Public Health Science, Iconic Open University Sokoto, Nigeria
*Corresponding Author:
Auwal Shehu Ali, School of Allied Health Sciences, Sharda University, Greater Noida, Uttar Pradesh, India., Email: auwalshehuali12@gmail.com
Abstract
Hypertension remains a paramount global health challenge characterized by its high prevalence and significant contribution to cardiovascular morbidity and mortality. As of 2025, approximately 1.56 billion adults worldwide are affected, with a disproportionate burden in low- and middle-income countries (LMICs). The multifactorial pathophysiology of hypertension involves genetic predispositions, neurohormonal dysregulation, endothelial dysfunction, and inflammatory processes. Advances in pharmacotherapy have introduced effective agents such as angiotensin-converting enzyme inhibitors, angiotensin receptor blockers, calcium channel blockers, and diuretics, which substantially reduce cardiovascular risks. However, global control rates remain suboptimal due to barriers including underdiagnosis, treatment non-adherence, limited healthcare access, and sociocultural factors. Patient-centered care models that emphasize education, lifestyle modification, individualized treatment, and multidisciplinary support demonstrate promising outcomes but require wider adoption, particularly in resource-limited settings. The review synthesizes current epidemiological trends, mechanistic insights, pharmacologic strategies, and patient-centered care approaches, highlighting the disparity in hypertension control across regions. It presents policy and healthcare system recommendations including national leadership, resource allocation, clinical guidelines, integrated health services, and population-level preventive measures. Emphasizing implementation science and health system strengthening, the study advocates for bridging gaps between pathophysiology, pharmacotherapy, and personalized care to reduce the cardiovascular disease burden. Collaborative global and local efforts aligned with sustainable development goals are critical to enhancing hypertension detection, treatment, and control, thereby reducing premature mortality from noncommunicable diseases.
Keywords
Downloads
-
1FullTextPDF
Article
Introduction
Hypertension, commonly known as high blood pressure, remains a foremost global health challenge and a leading modifiable risk factor for cardiovascular diseases (CVD), stroke, chronic kidney disease, and premature mortality worldwide. It also imposes substantial economic hardship through lost productivity and increased healthcare system expenses.1-2 In 2025, the estimated. number of adults living with hypertension is approximately 1.56 billion individuals, representing a 60% increase from previous decades.3-4 The global prevalence of hypertension is higher in low and middle-income countries (LMICs), where approximately two-thirds of affected individuals reside, compared to high-income countries (HICs).4-5 This disparity reflects differences in sociodemographic factors, healthcare infrastructure, lifestyle behaviors, and dietary patterns.
Despite a slight global decrease or stabilization in mean blood pressure levels in high-income regions over the past four decades, LMICs have experienced substantial increases in hypertension prevalence, attributable to urbanization, aging populations, physical inactivity, unhealthy diets (excess sodium and low potassium intake), and rising obesity rates.4 It is predicted that by 2025, over 1.5 billion adults worldwide will be hypertensive, with prevalence reaching 30-45% in adult populations and exceeding 60% among individuals aged 60 and above.3-6
The pathophysiology of hypertension is multifactorial, encompassing genetic predispositions and complex neuro-hormonal regulatory mechanism dysfunctions such as imbalances in the renin-angiotensin-aldosterone system, sympathetic nervous system over-activation, endothelial dysfunction, and oxidative stress.4 These mechanisms collectively increase peripheral vascular resistance and blood volume, leading to sustained elevated arterial pressure. However, disparities in access to diagnosis, treatment, and adherence to therapy are pronounced in LMICs, further complicating effective blood pressure management.7-8
Effective pharmacotherapy options, including angiotensin converting enzyme inhibitors (ACEIs), angiotensin receptor blockers (ARBs), calcium channel blockers, and diuretics, play a critical role in reducing blood pressure and minimizing CVD risks.1 Yet, suboptimal hypertension control persists globally, primarily due to underdiagnosis, poor treatment adherence, lack of access to medications, and sociocultural barriers, particularly in LMICs.4,9 Moreover, patient-centered care approaches integrating individualized treatment plans, lifestyle modifications, and multidisciplinary support have shown promising results but require broader implementation worldwide.
This review is especially relevant in 2025 in light of the recent WHO Global Hypertension Report 2024 and renewed global efforts aiming to reduce the hypertension burden and disparities. These developments underscore the urgent need for updated synthesis of epidemiology, pathophysiology, pharmacotherapies, and patient centered care strategies. By bridging scientific understanding with practical healthcare delivery, this review aims to identify actionable pathways for reducing the global hypertension burden and its associated inequities.
Methods
This review was conducted through a systematic and transparent approach following the Preferred Reporting Items for Systematic Reviews and Meta Analyses (PRISMA) 2022 guidelines, which provide a structured framework for literature identification, selection, and synthesis, to minimize bias and enhance reproducibility.10
Search Strategy
Comprehensive searches were carried out across multiple electronic databases, including PubMed, PubMed Central (PMC), Scopus, and Web of Science. Keywords and MeSH terms used included “global hypertension control,” “hypertension pathophysiology,” “pharmacotherapy of hypertension,” “patient-centered hypertension care,” and “blood pressure management.” Search filters were applied to retrieve articles published up to June 2025, including clinical trials, epidemiological studies, systematic reviews, guidelines, and intervention studies relevant to global hypertension control. Limiting the search period to 2020-2025 captures the most recent and relevant advances in hypertension research, including updates in diagnosis, treatment guidelines, and control strategies. This period reflects the impact of events like the COVID-19 pandemic on hypertension management and incorporates emerging therapies, digital health innovations, and evolving patient-centered care models. It also aligns with the latest global epidemiological data and policy changes, ensuring the review is timely and focused on current challenges and solutions in hyper-tension control. This precise timeframe maximizes relevance while maintaining comprehensive coverage of contemporary evidence and clinical practice updates.
Selection Criteria
Articles were included if they addressed at least one of the following domains:
I. Global or regional epidemiology of hypertension
II. Mechanistic insights into hypertension pathophysiology
III. Pharmacological therapies for hypertension and their global applicability
IV. Patient-centered care approaches and implementation strategies for hypertension control.
Additionally, government and non-government reports and grey literature relevant to hypertension control were included to enrich contextual evidence.
Exclusion criteria encompassed articles not in English, opinion pieces without empirical data, and studies unrelated to hypertension control or management.
Screening and Eligibility Assessment
Two independent reviewers screened titles and abstracts for relevance. Full-text versions of potentially eligible articles were then obtained and reviewed for inclusion based on the criteria. Discrepancies were resolved through discussion or consultation with a third reviewer. Quality assessment and risk of bias evaluation were conducted using established tools such as Cochrane risk of bias criteria and GRADE methodology to ensure the rigor of included studies.
Data Extraction and Synthesis
Data extracted included study design, population characteristics, geographic setting, interventions, outcome measures, and key findings. Qualitative synthesis was prioritized due to heterogeneity of study designs and endpoints.
PRISMA Flow Chart
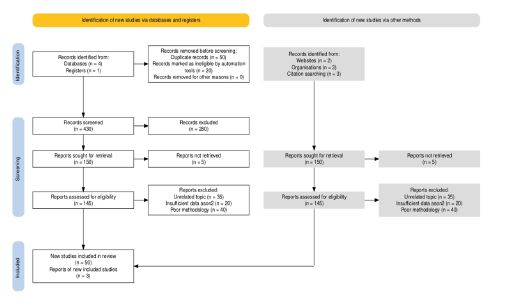
The study selection process is depicted in the PRISMA 2022 flow diagram (Figure 1).
Identification
- Databases used: 4 (PubMed, PubMed Central, Scopus, Web of Science)
- Registers searched: 1 (ClinicalTrials.gov)
- Organizations searched: 3 (WHO, Pan-African Society of Cardiology, American Heart Association websites)
- Other sources (websites, citations): 2 (Reference lists of included articles, Google Scholar)
- Total records identified from all sources: 500
- Duplicates removed: 50
- Records automatically excluded (e.g., by date or language filters): 20
Screening
- Records screened (titles and abstracts): 430
- Records excluded at screening: 280
Eligibility
- Reports sought for retrieval (full text assessed): 150
- Reports not retrieved (could not obtain full text): 5
- Reports assessed for eligibility: 145
- Reports excluded after full-text review: 95 (Reasons: unrelated topic, insufficient data, poor methodology)
Included
- Studies included in qualitative synthesis: 50
- New reports (additional relevant studies from citation tracking): 3
- Total studies/documents included: 53
Below is the PRISMA flow chart summarizing the listed information (Figure 1).
Discussion
Global Epidemiology and Country-Specific Examples
Hypertension is a major public health burden worldwide, with an estimated 1.56 billion adults affected as of 2025, a 60% increase from past decades.1 Above shows the global epidemiology chart summarizing vital information. The global prevalence is unevenly distributed, with LMICs bearing over two-thirds of the burden. The World Health Organization (WHO) reports 54% of hypertensive adults are diagnosed globally, 42% receive some form of treatment, but only 21% achieve adequate control (Figure 2).4,8
Country-specific data illustrate vast disparities. For example, Russia, Bulgaria, and Ukraine exhibit some of the highest age-adjusted hypertension-related death rates - 380.2, 680.8, and 540.2 deaths per 100,000 persons, respectively, indicating severe disease burden.9 In contrast, Nigeria shows a death rate of 53.1 per 100,000, reflecting a substantial but comparatively lower burden. Countries in the WHO Western Pacific and South-East Asia regions have experienced dramatic increases in hypertensive populations; in China, hypertensive adults increased from 144 million in 1990 to 346 million in 2019.5,8 India, similarly reports millions affected with inadequate control despite healthcare investments.4 High-income countries such as the United States and Germany report better awareness and control compared to LMICs, but still face challenges. The United States has an estimated 151 deaths per 100,000 population related to hypertension, with control rates improving but disparities persisting among underserved populations (Table 1).9
Trends in Hypertension and Cardiovascular Outcomes
Hypertension’s impact on cardiovascular morbidity and mortality remains profound. Elevated systolic blood pressure (≥110-115 mmHg) accounts for over 10 million deaths globally each year, mostly from ischemic heart disease and stroke.4 While some HICs have stabilized or slightly reduced mean blood pressures through effective public health interventions, many LMICs face rising trends due to urbanization and lifestyle changes that increase obesity, salt intake, and sedentary habits.8
Pharmacotherapy Utilization and Challenges
First-Line Agents
Pharmacological management of hypertension has evolved significantly, with established first-line agents. The primary classes of antihypertensive medications recommended as first-line agents include thiazide-type diuretics, calcium channel blockers (CCBs), angioten sin-converting enzyme inhibitors (ACEIs), and angiotensin receptor blockers (ARBs). Thiazide diuretics, particularly chlorthalidone and indapamide, are favoured for their proven efficacy in reducing cardiovascular disease risk and cost-effectiveness. ACEIs and ARBs are especially indicated for patients with chronic kidney disease, heart failure, or high cardiovascular risk due to their cardioprotective effects beyond blood pressure reduction. Calcium channel blockers are effective alternatives, particularly in nonblack populations, and they show beneficial outcomes in stroke prevention and heart failure reduction.11-13
Despite their proven efficacy, global hypertension control remains inadequate, particularly in LMICs. Key contributing factors to suboptimal outcomes include underdiagnosis, poor medication adherence, limited healthcare infrastructure, and high out-of-pocket costs for antihypertensive drugs. For instance, in SubSaharan Africa, significant challenges in medication availability and affordability restrict effective treatment delivery, leading to persistently high rates of uncontrolled hypertension.4
Emerging Therapies
Recent advances highlight novel agents and combination therapies aimed at improving blood pressure control and patient adherence. These include fixed low-dose triple single-pill combinations of telmisartan, amlodipine, and indapamide, which offer enhanced efficacy with simplified regimens. Additionally, emerging precision medicine approaches and digital health interventions are gaining traction for tailoring hypertension management. Ongoing research also focuses on novel pharmacological targets and the integration of lifestyle interventions with pharmacotherapy to optimize outcomes.12-13 Emerging pharmacotherapies offer promising new dimensions in hypertension management:
SGLT2 Inhibitors: Initially developed as glucose-lowering agents for type 2 diabetes, sodium-glucose cotransporter-2 (SGLT2) inhibitors have demonstrated consistent blood pressure-lowering effects alongside cardiovascular and renal protection benefits. These agents are especially advantageous for hypertensive patients with comorbid diabetes or heart failure, expanding therapeutic choices beyond traditional antihypertensives.3
Innovative Biologics: Cutting-edge biologic drugs targeting novel molecular pathways implicated in blood pressure regulation are under investigation, primarily for resistant or refractory hypertension. These include monoclonal antibodies and gene-modifying therapies that may pave the way for future personalized medicine approaches, though their clinical availability remains limited at present.2
Fixed-Dose Combination Therapy (Polypills): Polypills consolidate multiple antihypertensive medications into a single pill, markedly improving adherence by simplifying regimens and reducing pill burden. The World Health Organization and several hypertension guidelines increasingly endorse polypill strategies to optimize blood pressure control, particularly in resource-limited settings where medication access and compliance pose major hurdles.1-2
While beta blockers remain widely used, they are no longer recommended as first-line therapy for uncom-plicated primary hypertension due to less favourable outcome profiles, particularly concerning stroke prevention, compared to other drug classes. Patient centered care models that prioritize education, lifestyle modification, self-management support, and multidisciplinary healthcare team involvement have shown success in improving adherence and outcomes but require scaling, especially in LMIC contexts.4
Ultimately, leveraging these pharmacotherapy advancements in tandem with health system strengthening, policy support, and patient engagement is critical to closing the global hypertension control gap and reducing cardiovascular morbidity and mortality. Ongoing alongside implementation science will be pivotal in shaping future hypertension management paradigms.1- 4
Patient-Centered Care and Health System Interventions
Patient-centered models emphasize individual goal setting, education, lifestyle modification, and multidisciplinary involvement. Programs using community health workers to deliver culturally tailored education and medication adherence strategies have demonstrated improved blood pressure control in settings like rural India and parts of Latin America.14-15 Home blood pressure monitoring combined with digital health platforms enhances self-management and follow-up, though adoption remains variable globally.
Barriers remain high in LMICs where health infrastructure, medication affordability, and patient awareness limit care delivery. Health system strengthening and implementation science approaches are vital to close these gaps. The WHO Global Hypertension Report 2023 recommends multi-level strategies including policy interventions for salt reduction and universal health cover-age to mitigate these disparities.8
Conclusion
Hypertension remains a critical and escalating global health challenge with vast implications for cardiovascular disease, kidney disease, and premature mortality. The global hypertension burden has risen sharply to approximately 1.56 billion adults affected in 2025, predominantly impacting LMICs where detection, treatment, and control rates remain unacceptably low. Despite advancements in understanding hypertension pathophysiology and the development of effective pharmacotherapies including ACE inhibitors, ARBs, calcium channel blockers, and diuretics, suboptimal treatment adherence and healthcare access continue to impede successful blood pressure control worldwide. Patient-centered care strategies that integrate individualized treatment, risk factor modification, education, and team-based approaches show promise but require broader implementation, especially in resourceconstrained settings. Bridging the gaps between pathophysiology driven pharmacotherapy and patient centered care models, supported by health system strengthening and policy commitments, is essential to achieve meaningful reductions in the cardiovascular and economic burdens of hypertension globally.
Recommendations
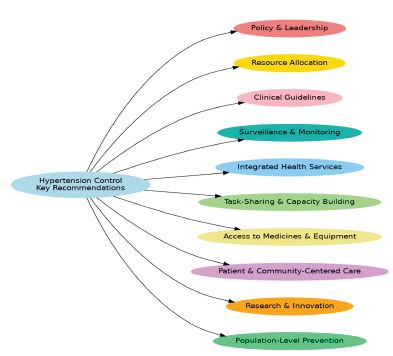
Building on the global evidence and the roadmap efforts such as the Pan-African Society of Cardiology (PASCAR) 10-point action plan, the following recommendations are proposed to advance hypertension control worldwide (Figure 3).
A. Policy and Leadership: Governments should exercise leadership by adopting and implementing national hypertension policies aligned with global targets for noncommunicable disease reduction (WHO, 2023).
B. Resource Allocation: Allocate sustainable funding and resources dedicated to early detection, treatment, and continuous control of hypertension within primary healthcare systems, with a focus on vulnerable and underserved populations.
C. Clinical Guidelines: Develop or adapt simple, evidence based hypertension management guidelines tailored to country-specific contexts to ensure standardized and effective care delivery (PASCAR Task Force, 2015).7
D. Surveillance and Monitoring: Establish robust systems for routine surveillance of hypertension prevalence, treatment, and control using standardized methodologies like the WHO Stepwise Approach (Page et al.,).6
E. Integrated Health Services: Integrate hypertension detection and management into existing health programs, such as HIV and tuberculosis clinics, to leverage resources and expand coverage.
F. Task-Sharing and Capacity Building: Promote task sharing with adequately trained community health workers and nurses to extend hypertension care beyond physicians, particularly in resource-limited settings.
G. Access to Medicines and Equipment: Ensure availability and affordability of essential antihypertensive medicines and validated blood pressure measuring devices at all healthcare levels.
H. Patient-Centered and Community-Based Care: Prioritize patient education, self-monitoring, lifestyle interventions, and culturally adapted care delivered through multidisciplinary teams to improve adherence and outcomes.
I. Research and Innovation: Invest in high-quality research to generate context-specific evidence guiding innovative hypertension care models and implementation strategies.
J. Population-Level Preventive Measures: Implement policies aimed at reducing dietary sodium intake, promoting physical activity, controlling obesity, and encouraging healthy diets at a population level.
Through concerted global and local actions embracing these recommendations, it is feasible to enhance hypertension detection and control, reduce cardiovascular morbidity and mortality, and close health disparities globally, contributing to achieving Sustainable Development Goal 3.4 to reduce premature mortality from noncommunicable diseases.7-8
Conflict of Interest
The authors declare no conflict of interest.
Acknowledgement
The authors extend sincere gratitude to all individuals and organizations whose support was integral to the successful completion of this study. We also acknowledge the assistance of healthcare professionals and community workers who facilitated data collection and provided critical insights. Appreciation is further extended to Professor Thimmasetty Juturu who made this research possible for his guidance and advices.
Supporting File
References
1. Bakris G, Hill M, Mancia G, et al. Achieving blood pressure goals globally: Five core actions for health-care professionals. J Hum Hypertens 2008;22(1): 63-70.
2. Bosworth HB, Olsen MK. Patient-centered hypertension management: Two team-based interventions. Fam Pract Manag 2023;30(4):15-22.
3. Kearney PM, Whelton M, Reynolds K, et al. Global burden of hypertension: Analysis of worldwide data. Lancet 2005;365(9455):217-23.
4. NCD Risk Factor Collaboration. The global epidemiology of hypertension: prevalence, awareness, treatment, and control. Nat Rev Nephrol 2020;16(4):223-37.
5. Özveren O. By 2025, hypertension patients are expected to reach 1.5 billion. Yeditepe Univ Hosp Health Guide [internet]. 2025 [cited 2025 August 10]. Available from: https://yeditepehastaneleri.com/en/health-guide/diseases-treatments/2025-hypertension-patients-are-expected-reach-15-billion
6. Page MJ, McKenzie JE, Bossuyt PM, et al. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. BMJ 2021;372:n71.
7. Pan-African Society of Cardiology (PASCAR) Task Force. Roadmap to achieve 25% hypertension control in Africa by 2025. Cardiovasc J Afr 2015;26(2):53-62.
8. World Health Organization. Hypertension. WHO fact sheet [internet]. 2023 [cited 2025 August 10]. Available from: https://www.who.int/news-room/fact-sheets/detail/hypertension
9. World Population Review. Hypertension rates by country 2025 [internet]. [cited 2025 August 10]. Available from: https://worldpopulationreview.com/country-rankings/hypertension-rates-by-country
10. Haddaway NR, Page MJ, Pritchard CC, et al. PRIS-MA2020: an R package and Shiny app for producing PRISMA 2020-compliant flow diagrams, with interactivity for optimized digital transparency and open synthesis. Campbell Syst Rev 2022;18:e1230.
11. American Heart Association. Professional Heart Daily. 2025 High Blood Pressure Guideline. [internet] 2025 [cited 2025 August 20]. Available from: https://professional.heart.org/en/science-news/2025-high-blood-pressure-guideline
12. DynaMed. Hypertension Medication Selection and Management. EBSCO Information Services. [internet] 2025 [cited 2025 September 16]. Available from: https://www.dynamed.com/management/hypertension-medication-selection-and-management
13. Khalil H, Zeltser R. Antihypertensive medications. StatPearls [internet]. Treasure Island (FL): StatPearls Publishing; 2023 [cited 2025 September 16]. Available from: https://www.ncbi.nlm.nih.gov/ books/NBK554579/
14. Smith DK. Managing hypertension using combination therapy. Am Fam Physician 2020;101(6): 341-8.
15. Riddell MA, Harshfield EL, Bazzano LA, et al. ASHA-led community-based groups to support control of hypertension in rural India are feasible and potentially scalable. Front Med (Lausanne) 2021;8:771822.